Healthy fingernails are not only aesthetically pleasing but also reflect the overall well-being of an individual. However, it’s not uncommon to experience various abnormalities in the appearance and texture of our nails. These abnormalities can range from discoloration and pitting to ridges and brittleness, and they often indicate underlying health issues or external factors affecting nail health.

In this blog post, we will explore the most common fingernail abnormalities, their causes, and potential treatments. By understanding these abnormalities, you can better recognize any changes in your nails and take appropriate steps to maintain healthy and beautiful nails.
#1: Discoloration
Discoloration of the fingernails can be concerning and may indicate an underlying issue affecting nail health. Let’s explore some common types of nail discoloration and their potential causes.
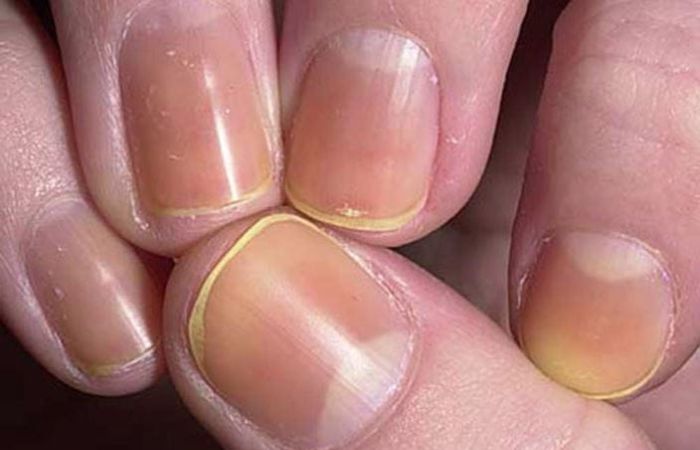
Yellow Nails
Yellow nails are a commonly observed discoloration that can be attributed to various factors. One of the main causes is nail fungus, known as onychomycosis. Fungal infections can result in a yellowish or brownish tint to the nails, along with thickening and brittleness. Other causes of yellow nails include smoking, frequent use of dark nail polish, and certain medical conditions such as diabetes and lung disease.
To prevent and treat yellow nails, it is crucial to maintain good nail hygiene. Keep your nails clean and dry, avoid prolonged exposure to moisture, and wear protective gloves when working with harsh chemicals. If a fungal infection is suspected, seeking medical attention for proper diagnosis and treatment is essential.
Blue Nails
The presence of a bluish tint on the nails can indicate a lack of oxygen supply or poor circulation. Medical conditions such as Raynaud’s disease, which causes blood vessel spasms, can result in blue nails. In some cases, blue nails may also be a symptom of respiratory or cardiovascular disorders. If you notice persistent blue discoloration of your nails, it is advisable to consult a healthcare professional for an evaluation and appropriate management.
Maintaining healthy nail color can be achieved by adopting a balanced lifestyle that includes regular exercise, a well-rounded diet, and avoiding habits such as smoking that can negatively impact circulation.
White Spots on Nails
White spots or dots on the nails are a common occurrence and are usually harmless. These spots, known as leukonychia, can be caused by minor injuries to the nail bed or excessive pressure on the nails. They can also be a result of nutrient deficiencies, particularly zinc or calcium.
#2: Nail Pitting
Nail pitting refers to the presence of small depressions or tiny dents on the surface of the fingernails. This abnormality can be an indicator of an underlying condition affecting the nail matrix, which is responsible for the production of nail cells. Let’s delve into the details of nail pitting, its associated conditions, and available management strategies.
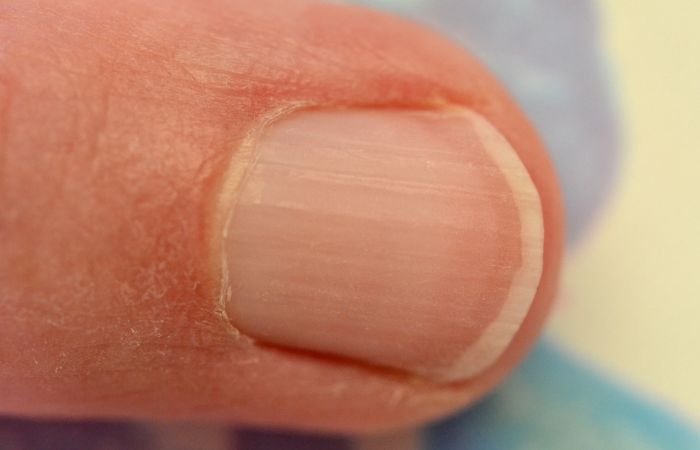
Definition and Appearance
Nail pitting manifests as small, shallow depressions or indentations on the nails. These pits can vary in size and depth, ranging from barely noticeable to more pronounced dents. Nail pitting is often observed on multiple nails and can affect both the fingernails and toenails.
Conditions Associated with Nail Pitting
Psoriasis
Psoriasis, an autoimmune skin disorder, is one of the primary causes of nail pitting. Individuals with psoriasis may experience pitting along with other nail abnormalities such as crumbling, thickening, and discoloration. Psoriatic nail changes often coincide with skin lesions and joint inflammation.
Alopecia Areata
Alopecia areata, an autoimmune condition that causes hair loss, is also frequently associated with nail pitting. Nail changes may occur alongside patchy hair loss and typically affect the toenails as well.
Other Autoimmune Disorders
Nail pitting can sometimes be linked to other autoimmune disorders such as rheumatoid arthritis and systemic lupus erythematosus (SLE). These conditions can affect multiple systems in the body, including the nails.
Managing and Treating Nail Pitting
While nail pitting itself may not be treatable, managing the underlying condition contributing to it can help improve the appearance of the nails. Here are some strategies for managing nail pitting:
Medical Interventions
Consulting a dermatologist or rheumatologist can help diagnose and manage underlying conditions associated with nail pitting. Treatment options may include topical medications, systemic therapies, or immunosuppressants, depending on the specific condition.
Home Remedies and Lifestyle Changes
While home remedies cannot cure nail pitting, they can support overall nail health. These include keeping the nails clean and dry, avoiding trauma to the nails, and using moisturizers to prevent dryness. Wearing gloves while performing household chores or working with chemicals can also protect the nails from further damage.
#3: Beau’s Lines
Beau’s lines are a distinctive type of fingernail abnormality characterized by horizontal depressions or grooves that traverse the nail plate. These lines can appear on one or multiple nails and are often indicative of an underlying health condition or stress on the body. Let’s delve into the details of Beau’s lines, their causes, and potential treatment options.
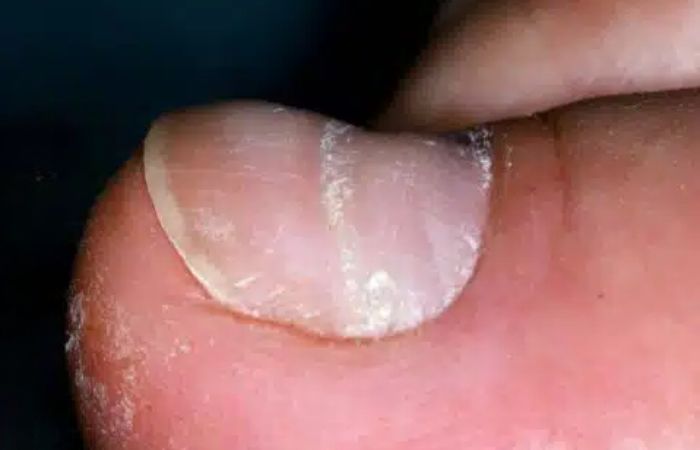
Understanding Beau’s Lines
Beau’s lines are named after the French physician Joseph Honoré Simon Beau, who first described this nail abnormality. These lines are typically transverse, running horizontally across the nails. They can be seen as indentations or grooves that extend from one side of the nail to the other. Beau’s lines can affect both fingernails and toenails.
Causes and Contributing Factors
Nutritional Deficiencies
Severe malnutrition or deficiencies in essential nutrients, particularly zinc, iron, and proteins, can lead to the development of Beau’s lines. Inadequate intake or absorption of these nutrients can impact the growth and formation of healthy nail cells.
Trauma or Injury
Significant physical trauma or injury to the nail matrix can result in the formation of Beau’s lines. This can occur due to accidents, surgeries, or habitual behaviors like nail biting or excessively aggressive manicuring.
Certain Medical Conditions
Beau’s lines can also be associated with various systemic conditions, including uncontrolled diabetes, peripheral vascular disease, chemotherapy, and certain infections. These conditions can disrupt the normal nail growth process and lead to the formation of horizontal lines.
Treatment and Prevention Strategies
Improving Overall Nail Health
Maintaining good nail hygiene and adopting healthy habits can contribute to the prevention and management of Beau’s lines. This includes keeping the nails clean, avoiding excessive trauma or injury, and moisturizing the nails and cuticles regularly to prevent dryness.
Addressing Underlying Causes
Identifying and treating the underlying condition contributing to Beau’s lines is crucial for optimal management. If nutritional deficiencies are suspected, consulting with a healthcare professional or registered dietitian can help develop a well-balanced diet plan or recommend appropriate supplements. For systemic conditions, working closely with a healthcare provider to manage the underlying condition can potentially improve the appearance of Beau’s lines.
#4: Clubbing
Clubbing refers to an abnormality in the shape and texture of the fingernails and is characterized by the enlargement of the fingertips, rounding of the nail bed, and a spongy or soft sensation when palpated. It is often associated with underlying medical conditions that affect the cardiovascular or respiratory systems. Let’s explore the details of clubbing, its associated conditions, and how to recognize and manage this fingernail abnormality.
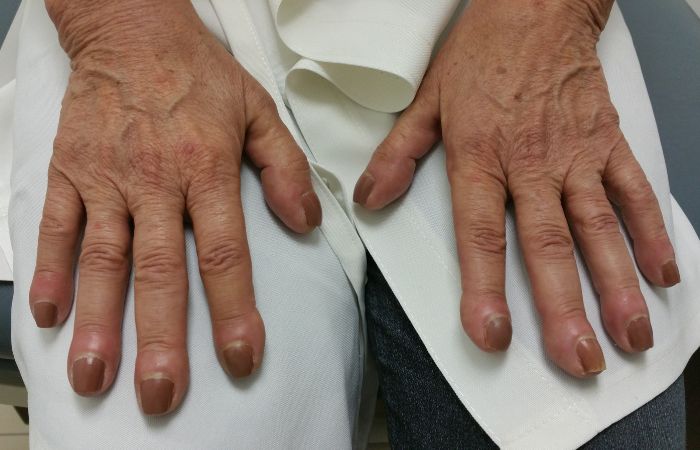
What is Nail Clubbing?
Nail clubbing is a condition in which the fingertips and nails undergo changes in their shape and structure. Instead of the normal angle between the nail and the nail bed, the nails become rounded or dome-shaped. The nail bed itself may feel spongy when pressed, and the nails may appear to “float” or detach from the underlying tissue.
Associated Medical Conditions
Lung Diseases
Clubbing is commonly observed in individuals with chronic lung diseases, such as chronic obstructive pulmonary disease (COPD), bronchiectasis, or lung cancer. It can be a result of chronic hypoxia (low oxygen levels) in the blood vessels of the fingertips.
Cardiovascular Disorders
Certain heart and circulatory conditions, including congenital heart defects, endocarditis, and cyanotic heart disease, can also cause nail clubbing. In these cases, inadequate oxygenation of the blood may lead to changes in the nail bed and nail structure.
Recognizing and Evaluating Clubbed Nails
Clubbing is usually a progressive condition that develops over time. Early signs may include softening of the nail bed and a loss of the normal angle between the nail and finger. As the condition advances, the nails become more rounded and the fingertips may appear enlarged. Diagnostic tests such as imaging studies, blood tests, and pulmonary function tests may be conducted to evaluate the underlying cause of clubbing.
Management and Medical Interventions
The primary approach to managing clubbing involves addressing and treating the underlying condition causing it. For lung diseases, treatment focuses on improving respiratory function and oxygenation, which may include medication, oxygen therapy, and pulmonary rehabilitation. In cases of cardiovascular disorders, managing the heart condition and optimizing blood flow and oxygenation are key.
In severe cases where clubbing causes significant discomfort or interferes with hand function, surgical intervention may be considered to reshape the fingertips and nails. However, this is typically reserved for exceptional cases.
#5: Koilonychia (Spoon Nails)
Koilonychia, commonly known as spoon nails, is a fingernail abnormality characterized by a concave shape, resembling a spoon. The nails appear to be scooped out, with a depression in the center that can hold a drop of liquid. Let’s explore the details of koilonychia, its potential causes, and available treatment options.
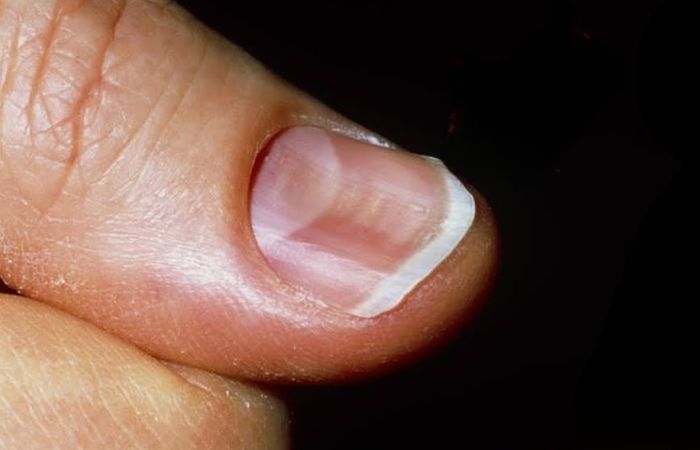
Characteristics of Spoon Nails
Spoon nails, or koilonychia, have a distinct appearance that sets them apart from normal, healthy nails. They are characterized by a concave shape, curving upwards at the edges and creating a depression in the middle of the nail. This indentation is often deep enough to hold a small drop of liquid, such as water.
Potential Causes
Iron Deficiency Anemia
One of the most common causes of koilonychia is iron deficiency anemia. Inadequate iron levels in the body can affect the growth and structure of the nails, leading to spoon-shaped deformity. Iron deficiency anemia is often accompanied by other symptoms such as fatigue, weakness, and pale skin.
Hypothyroidism
Underactive thyroid gland or hypothyroidism can also contribute to the development of spoon nails. The thyroid hormone plays a crucial role in nail health, and its deficiency can cause changes in the nail structure, including koilonychia.
Nail Trauma
Repeated trauma or injury to the nail bed can result in koilonychia. This can occur due to activities or occupations that involve frequent pressure or impact on the fingertips.
Treatment and Self-Care Measures
Addressing Underlying Causes
Treating the underlying condition that is causing koilonychia is essential for managing spoon nails. For example, in cases of iron deficiency anemia, iron supplementation may be recommended after a thorough evaluation by a healthcare professional. Similarly, managing hypothyroidism with appropriate medications can help improve nail health.
Nail Care
Taking good care of the nails is essential for managing koilonychia. This includes keeping the nails well-moisturized, protecting them from excessive exposure to water or chemicals, and avoiding trauma or injury. Wearing gloves while doing household chores or using protective measures in occupational settings can help prevent further damage to the nails.
#6: Onycholysis
Onycholysis is a fingernail abnormality characterized by the separation of the nail plate from the nail bed. This condition can cause the affected portion of the nail to appear white, yellow, or greenish, and it may be accompanied by pain or discomfort. Let’s delve into the details of onycholysis, its common causes, and available treatment options.
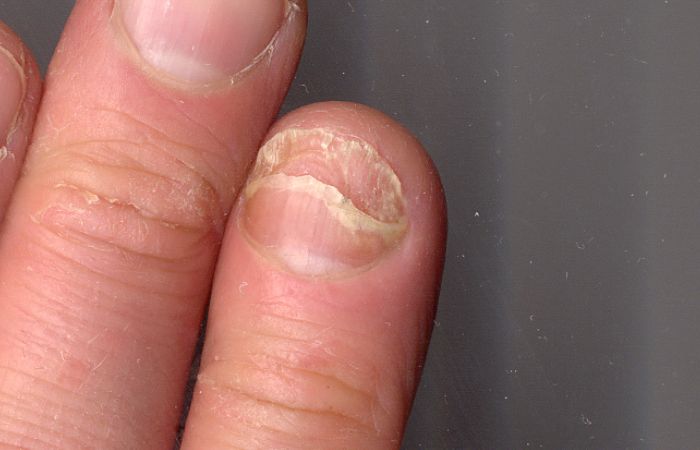
Definition and Appearance
Onycholysis refers to the detachment of the nail plate from the underlying nail bed. This separation often starts at the tip of the nail and gradually progresses towards the base. As a result, the affected portion of the nail appears discolored, with a visible gap between the nail and the nail bed. The color of the detached area can vary, ranging from white to yellow or even greenish, depending on the underlying cause.
Common Causes of Onycholysis
Trauma
Physical trauma or injury to the nail, such as excessive force, repetitive rubbing, or prolonged exposure to moisture, can lead to onycholysis. This can occur from activities such as typing, playing musical instruments, or wearing tight-fitting shoes.
Infection
Fungal or bacterial infections can also cause onycholysis. Fungal infections, known as onychomycosis, can lead to the separation of the nail plate from the nail bed. Bacterial infections, such as pseudomonas infection, can cause greenish discoloration and subsequent detachment of the nail.
Chemical Exposure
Exposure to certain chemicals, including household cleaning agents, solvents, or nail products containing harsh chemicals, can cause onycholysis. Prolonged or repeated contact with these substances can weaken the nail structure and result in separation from the nail bed.
Treatment Options and Prevention Tips
Medical Interventions
In cases of severe or persistent onycholysis, medical intervention may be necessary. Treatment options can include antifungal or antibacterial medications for infections, topical or oral treatments for fungal infections, and professional removal of the detached portion of the nail if required.
Self-Care Measures
Practicing good nail hygiene is crucial for managing and preventing onycholysis. This includes keeping the nails clean and dry, avoiding excessive trauma or injury to the nails, and protecting them from chemical exposure by wearing gloves. It is also important to avoid picking or pulling at the detached portion of the nail, as this can further aggravate the condition.
#7: Nail Ridges
Nail ridges are a common fingernail abnormality characterized by raised lines or ridges that run vertically or horizontally along the surface of the nails. While nail ridges are often harmless, they can sometimes be a sign of an underlying health condition or aging. Let’s explore the details of nail ridges, their types, potential causes, and management strategies.
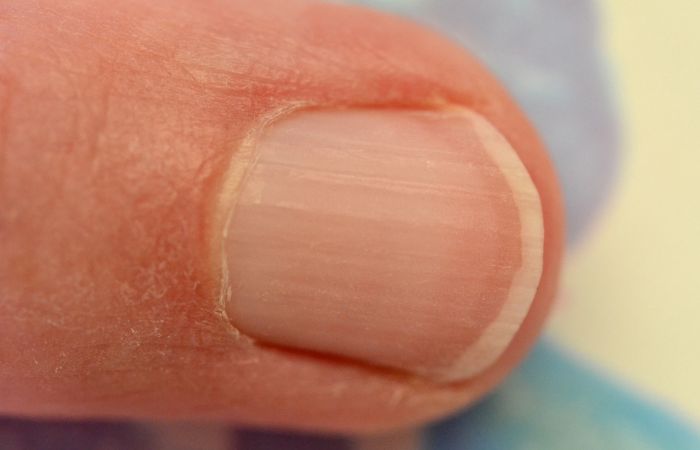
Understanding Nail Ridges
Nail ridges are elevated lines or grooves that can appear vertically or horizontally on the nails. They may vary in depth and severity, ranging from barely noticeable to more pronounced ridges that extend the entire length of the nail. Nail ridges can affect one or multiple nails.
Types of Nail Ridges
Vertical Ridges
Vertical ridges are the most common type of nail ridges. They run from the base of the nail towards the tip and are generally harmless. Vertical ridges are often associated with aging and are more commonly observed in older individuals. As we age, the rate of cell turnover in the nail matrix slows down, leading to the formation of ridges.
Horizontal Ridges
Horizontal ridges, also known as Beau’s lines, differ from vertical ridges in their orientation. They appear as transverse lines that extend horizontally across the nails. Horizontal ridges can be a sign of underlying health issues or trauma to the nail matrix, such as severe illness, nutritional deficiencies, or injury.
Possible Causes and Risk Factors
Aging
Vertical ridges are a natural part of the aging process. As we grow older, the production of new nail cells slows down, leading to the formation of ridges. Vertical ridges are generally harmless and do not require specific treatment.
Nutritional Deficiencies
Certain nutrient deficiencies, such as deficiencies in vitamins, minerals (like zinc), or proteins, can contribute to the development of nail ridges. Inadequate intake or absorption of these nutrients can impact nail health and lead to the formation of ridges.
Trauma or Injury
Physical trauma or injury to the nails can result in the formation of horizontal ridges. This can occur due to accidents, surgeries, or habitual behaviors like nail biting or aggressive manicuring.
Managing and Improving Nail Ridges
Balanced Diet
Consuming a well-balanced diet that includes essential vitamins, minerals, and proteins can support overall nail health and minimize the occurrence of ridges. Foods rich in biotin, vitamin E, and omega-3 fatty acids can be particularly beneficial.
Nail Care
Practicing good nail care can help improve the appearance and health of the nails. This includes keeping the nails clean, moisturized, and protected from excessive trauma or injury. Avoiding harsh chemicals and wearing gloves when performing household chores or working with chemicals can also prevent damage to the nails.
#8: Nail Fungus
Nail fungus, medically known as onychomycosis, is a common fungal infection that affects the nails, particularly the toenails. It can cause the nails to become discolored, thickened, brittle, and distorted. Nail fungus can be persistent and challenging to treat. Let’s explore the details of nail fungus, its signs and symptoms, risk factors, prevention, and available treatment options.
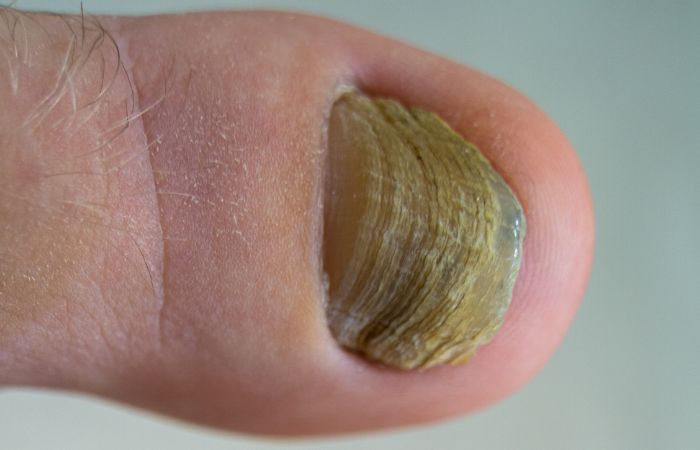
Introduction to Nail Fungus
Nail fungus is a fungal infection that primarily affects the nails, including both fingernails and toenails. It is most commonly caused by dermatophyte fungi, but other types of fungi can also be responsible. The infection typically starts at the edge of the nail and gradually spreads to the entire nail, leading to various characteristic changes in its appearance and texture.
Signs and Symptoms of Nail Fungal Infection
The signs and symptoms of nail fungus may vary depending on the severity and duration of the infection. Common indications of nail fungal infection include:
- Discoloration: Infected nails may turn yellow, brown, or white. In some cases, the color may appear green due to the presence of certain types of fungi.
- Thickened Nails: Fungal infection can cause the nails to thicken and become abnormally shaped. The nails may appear distorted and lose their natural smoothness.
- Brittle or Crumbly Texture: Infected nails often become brittle, fragile, and prone to crumbling or breaking.
- Nail Lifting: The nail may start to separate from the nail bed, a condition known as onycholysis. This can cause discomfort and create a gap between the nail and the nail bed.
Risk Factors and Prevention
Several factors increase the risk of developing nail fungus. These include:
- Warm and Moist Environments: Fungi thrive in warm, moist environments such as public swimming pools, locker rooms, and communal showers. Avoid walking barefoot in such areas to minimize the risk of infection.
- Poor Nail Hygiene: Inadequate nail hygiene, including not keeping the nails clean and trimmed, can create an environment conducive to fungal growth.
- Damaged Nails: Nails that are injured or have undergone trauma are more susceptible to fungal infections. It is important to take precautions to protect the nails from injury.
- Weakened Immune System: Individuals with weakened immune systems, such as those with diabetes, HIV/AIDS, or autoimmune disorders, are more susceptible to nail fungus.
Taking preventive measures can help reduce the risk of nail fungal infections. These include keeping the nails clean and dry, wearing moisture-wicking socks and breathable shoes, using antifungal powders or sprays in shoes, and avoiding sharing personal items such as nail clippers or files.
Treatment Options and Home Remedies
Treating nail fungus can be challenging, and it often requires a combination of approaches. Treatment options include:
- Topical Antifungal Medications: Over-the-counter or prescription-strength antifungal creams, lotions, or nail lacquers can be applied directly to the affected nails to combat the infection.
- Oral Antifungal Medications: In severe cases or when topical treatments are not effective, oral antifungal medications may be prescribed. These medications target the infection from within the body.
- Laser or Light Therapy: Certain laser or light therapies can help eliminate fungal infections by targeting the fungi without causing damage to the surrounding tissues.
Home remedies such as vinegar soaks, tea tree oil, or hydrogen peroxide are sometimes used as adjunct treatments. However, their effectiveness varies, and it is important to consult with a healthcare professional for proper diagnosis and guidance on appropriate treatment options.
#9: Ingrown Nails
Ingrown nails, also known as onychocryptosis, occur when the edges of the nails grow into the surrounding skin, causing pain, inflammation, and potential infection. This common nail condition often affects the toenails, especially the big toe. Let’s explore the details of ingrown nails, their symptoms, causes, treatment options, and preventive measures.
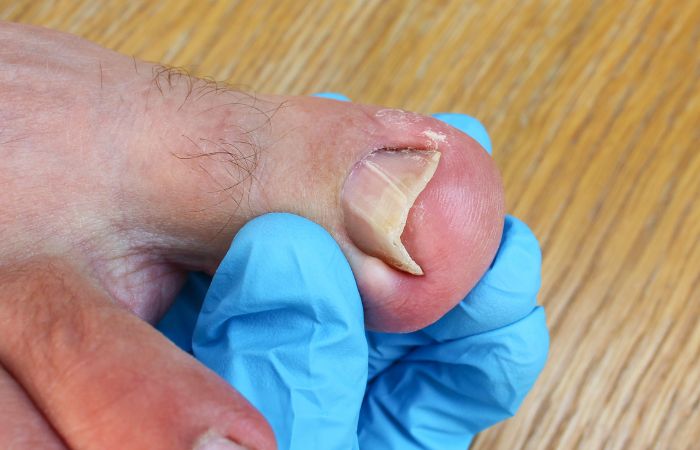
Definition and Common Causes
Ingrown nails develop when the corners or sides of the nails curve and penetrate the adjacent skin. Several factors contribute to the development of ingrown nails, including:
- Improper Nail Trimming: Nails that are trimmed too short or rounded off at the corners can encourage the nail to grow into the skin.
- Tight-Fitting Shoes: Wearing shoes that are too tight or narrow can compress the toes, pushing the nails into the surrounding skin.
- Trauma or Injury: Stubbing the toe or experiencing repetitive trauma to the nails can cause them to grow abnormally and become ingrown.
- Genetic Predisposition: Some individuals have a genetic predisposition to ingrown nails, making them more prone to developing this condition.
Symptoms and Complications
Ingrown nails can cause a range of symptoms, including:
- Pain and Tenderness: Ingrown nails often cause pain and tenderness along the affected nail edges.
- Swelling and Redness: The surrounding skin may become swollen, red, and inflamed.
- Infection: If left untreated, ingrown nails can lead to infection, which may result in pus formation, increased pain, and additional complications.
Treating and Preventing Ingrown Nails
Professional Care
For mild cases, home remedies such as warm soaks, gentle lifting of the nail, and applying antibiotic ointments can help alleviate symptoms and promote healing. However, severe or recurrent ingrown nails may require professional care from a podiatrist or healthcare provider. They can provide specialized treatment, such as partial nail avulsion (removal of part of the nail) or complete nail avulsion, to permanently address the ingrown nail and prevent future occurrences.
At-Home Remedies and Prevention
To prevent ingrown nails, it is important to practice proper nail care, including:
- Trimming Nails Correctly: Trim nails straight across and avoid rounding the corners. Cutting nails too short increases the risk of ingrown nails.
- Wearing Proper Footwear: Choose shoes that fit properly, allowing enough space for the toes to move comfortably.
- Protecting the Feet: When participating in activities that may cause trauma to the toes, such as sports or manual labor, wear protective footwear.
- Maintaining Good Foot Hygiene: Keep feet clean and dry, and avoid excessive moisture that can soften the nails and make them more prone to ingrowth.
#10: Brittle Nails
Brittle nails are a common nail abnormality characterized by nails that are weak, fragile, and prone to splitting, peeling, or breaking. This condition can be frustrating and affect the overall appearance and strength of the nails. Let’s explore the details of brittle nails, potential causes, and tips for improving nail strength and resilience.
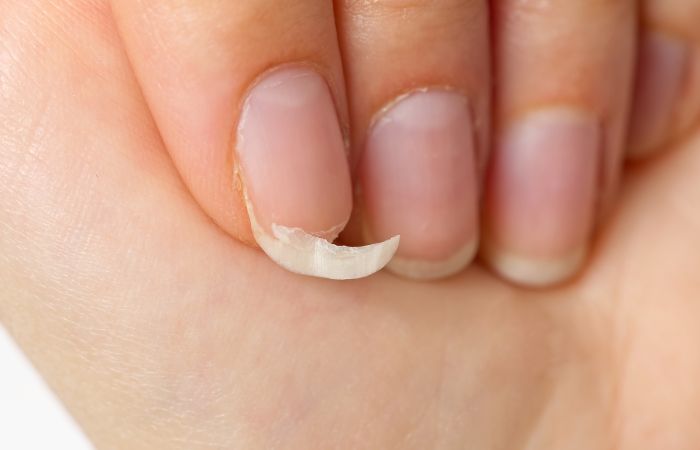
Identifying Brittle Nails
Brittle nails have a fragile texture and are more prone to breakage than healthy nails. They may appear dry, dull, and have a tendency to split or peel at the edges. Brittle nails can affect both fingernails and toenails, making them susceptible to damage and making it difficult to grow nails to the desired length.
Factors Contributing to Brittle Nails
Several factors can contribute to the development of brittle nails, including:
Aging
As we age, the nails naturally become more brittle and prone to dryness. The decreased production of natural oils and reduced blood circulation to the nail beds contribute to this change.
Nutritional Deficiencies
A lack of essential nutrients, such as biotin, vitamins A and C, iron, and zinc, can lead to brittle nails. These nutrients play a vital role in maintaining healthy nail structure and growth.
Excessive Water or Chemical Exposure
Excessive and prolonged exposure to water, such as frequent handwashing or submerging the nails in water for long periods, can weaken the nails. Similarly, frequent exposure to chemicals or harsh cleaning agents without proper hand protection can also contribute to nail brittleness.
Tips for Improving Nail Strength and Resilience
Balanced Diet
Consuming a well-rounded diet that includes essential nutrients can promote nail health and combat brittleness. Foods rich in biotin, vitamins A and C, iron, and zinc, such as fruits, vegetables, lean proteins, and whole grains, can support nail strength.
Moisturizing and Hydration
Keep the nails and cuticles well-moisturized by regularly applying nourishing creams or oils. Additionally, hydrate the body adequately by drinking enough water to maintain overall nail and skin health.
Protective Measures
Wear gloves when performing household chores or working with water or chemicals to protect the nails from damage. This is particularly important when handling cleaning agents or engaging in activities that expose the nails to excessive moisture.
Avoid Harsh Nail Care Practices
Limit the use of nail polish removers containing harsh chemicals, as they can dry out the nails. Instead, choose acetone-free removers or opt for gentle, non-acetone formulas.
Conclusion
Taking care of your fingernails goes beyond just keeping them clean and well-groomed. Your nails can provide valuable insights into your overall health and well-being. By being aware of common fingernail abnormalities and their causes, you can identify potential health issues early on and seek appropriate medical attention.
Remember to practice good nail hygiene, nourish your nails with a balanced diet, and protect them from excessive trauma or chemical exposure. By maintaining healthy nail habits and promptly addressing any abnormalities, you can enjoy strong, beautiful nails that serve as a reflection of your overall health.