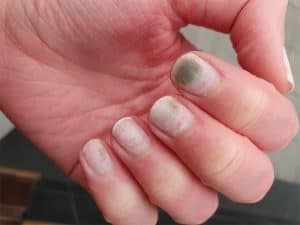
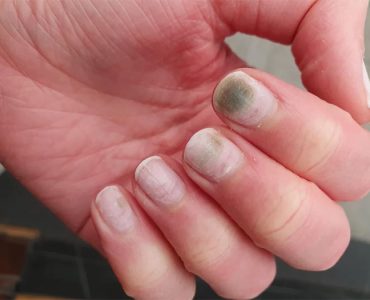
Are you experiencing discomfort, discoloration, or a foul odor emanating from your nails? If so, you may be dealing with a common nail problem. However, pinpointing the exact cause can be challenging, as nail fungus and bacterial infections share similar symptoms.

It’s crucial to distinguish between the two to ensure proper treatment and prevent the condition from worsening. In this blog post, we will explore the differences between nail fungus and bacterial infections, shedding light on their causes, symptoms, and treatment options. By understanding these distinctions, you can take the necessary steps to restore the health and appearance of your nails.
Differentiating Factors: Nail Fungus vs. Bacterial Infections
When it comes to nail problems, distinguishing between nail fungus and bacterial infections is crucial for effective treatment and management. While both conditions may exhibit similar symptoms, there are distinct factors that can help differentiate between the two. By understanding these differentiating factors, individuals can seek appropriate care and prevent the condition from worsening. Let’s delve into the key aspects that set nail fungus apart from bacterial infections.
Nail Appearance and Texture
One of the primary factors in distinguishing between nail fungus and bacterial infections lies in the appearance and texture of the affected nails. Taking a close look at the nails can provide valuable insights into the underlying cause of the problem.
Nail Fungus
When dealing with nail fungus, the affected nail often exhibits distinct changes in its appearance and texture. Discoloration is a common characteristic, with the nail taking on a yellow or brownish hue. In some cases, the discoloration may spread across the entire nail bed, making it visibly different from the healthy nails.
Another telltale sign of nail fungus is the thickening of the affected nail. The nail may become noticeably thicker than usual, resulting in an abnormal and often uncomfortable sensation. As the infection progresses, the texture of the nail may become brittle or crumbly, making it prone to breakage. Individuals may find that their nails become difficult to trim or that they easily chip or peel.
Bacterial Infections
In contrast, bacterial infections of the nails often present with distinct visual cues. Redness and swelling around the nail bed are characteristic signs of a bacterial infection. The affected area may appear inflamed, tender to the touch, and may feel warm or hot. This inflammation is a result of the body’s immune response to the bacterial invasion.
Bacterial infections can also lead to the formation of pus-filled pockets or abscesses. These pockets may develop around the edges of the nail or within the nail bed itself. They can cause considerable pain and discomfort, and in some cases, may even lead to the separation or detachment of the nail from the nail bed.
Read This Next:
Associated Symptoms and Discomfort
In addition to changes in nail appearance and texture, associated symptoms and discomfort can provide further insights into whether the nail problem is caused by nail fungus or a bacterial infection. Understanding these additional symptoms can aid in distinguishing between the two conditions.
Nail Fungus
Nail fungus can be accompanied by various symptoms and discomfort. Individuals with nail fungus may experience a persistent foul odor emanating from the affected nail. This odor is often described as unpleasant and can be a source of embarrassment and self-consciousness.
Some individuals may also notice an increase in nail brittleness or a crumbly texture. This can make the nails more prone to breakage, leading to further discomfort. In some cases, the affected nail may become lifted or separated from the nail bed, causing sensitivity and making it more susceptible to injury.
Bacterial Infections
Bacterial infections of the nails can present with distinct symptoms and discomfort. The most common symptoms include redness, swelling, and tenderness around the affected nail. These signs indicate an active inflammatory response by the body’s immune system.
Bacterial infections can also cause pain and discomfort, especially when pressure is applied to the affected area. The presence of pus-filled pockets or abscesses can result in throbbing or pulsating pain. If left untreated, the infection may spread, leading to worsening symptoms and potential complications.
Diagnostic Techniques
Accurate diagnosis is essential in distinguishing between nail fungus and bacterial infections. Healthcare professionals employ various diagnostic techniques to identify the underlying cause of the nail problem and determine the most appropriate treatment approach.
Clinical Examination
A healthcare professional will begin the diagnostic process by conducting a thorough clinical examination of the affected nails. They will observe the nail appearance, texture, and any associated symptoms. By visually assessing the nails and discussing the patient’s medical history and symptoms, the healthcare provider can gather important information for further evaluation.
Nail Scrapings and Cultures
To confirm the presence of nail fungus, the healthcare professional may collect nail scrapings for laboratory analysis. These samples are examined under a microscope or sent to a laboratory for fungal culture. This process helps identify the specific type of fungus responsible for the infection, aiding in the selection of appropriate antifungal treatment.
In the case of bacterial infections, a similar procedure may be performed. Nail scrapings or swabs are obtained to collect samples of the infected area. These samples are then cultured in a laboratory to identify the specific bacteria causing the infection. This information is crucial in determining the most effective antibiotic treatment.
Other Diagnostic Tests
In certain cases, additional diagnostic tests may be utilized to differentiate between nail fungus and bacterial infections. For instance, a potassium hydroxide (KOH) test may be performed on nail clippings to help detect the presence of fungal elements. This test involves dissolving the nail sample in KOH solution and examining it under a microscope.
In more complex or challenging cases, a biopsy may be recommended. A small sample of the affected nail or surrounding tissue is surgically removed and examined under a microscope. This procedure helps rule out other potential causes and provides a definitive diagnosis.
Contagiousness and Spread
Understanding the contagiousness and spread of nail fungus and bacterial infections is crucial in preventing their transmission and managing the condition effectively. While both conditions can be contagious to some extent, there are important distinctions to consider.
Nail Fungus
Nail fungus is typically contagious and can spread from person to person or from one area of the body to another. Fungal spores can survive in warm, moist environments such as public swimming pools, locker rooms, and communal showers. Sharing personal items like nail clippers, files, or shoes can also contribute to the spread of nail fungus.
It’s important to note that not everyone who comes into contact with fungal spores will develop a nail infection. Certain factors, such as a weakened immune system, frequent exposure to moisture, or minor nail trauma, can increase the risk of infection. However, taking preventive measures such as practicing good foot hygiene, avoiding walking barefoot in public areas, and refraining from sharing personal items can significantly reduce the likelihood of contracting or spreading nail fungus.
Bacterial Infections
Bacterial nail infections are typically not as contagious as fungal infections. While they can be transmitted from person to person, the risk of spread is generally lower. Bacterial infections of the nails often occur due to an existing injury or trauma to the nail, providing an entry point for bacteria to invade.
Proper wound care and hygiene are essential in preventing the spread of bacterial infections. Keeping the affected area clean, avoiding exposure to dirty or contaminated environments, and refraining from sharing personal items can help minimize the risk of transmission.
Read This Next:
Response to Treatment
Understanding how nail fungus and bacterial infections respond to treatment is crucial in determining the most effective approach for managing these conditions. While both conditions require intervention, the response to treatment can vary.
Nail Fungus
Treating nail fungus can be a lengthy process as the infection often resides deep within the nail and is challenging to reach. Topical antifungal medications, such as creams, ointments, or nail lacquers, are commonly used for mild to moderate cases. These medications are applied directly to the affected nail and surrounding skin.
For more severe or persistent cases, oral antifungal medications may be prescribed. These medications work systemically, targeting the fungal infection from within the body. It’s important to note that oral antifungals often require a longer treatment duration and regular monitoring by a healthcare professional due to potential side effects.
In some cases, laser treatment or surgical intervention may be recommended for stubborn or recurrent nail fungus. Laser therapy targets and destroys the fungus while preserving the healthy tissue. Surgical options, such as nail removal, may be considered in severe cases or when other treatment methods have been ineffective.
The response to treatment for nail fungus can vary among individuals. It’s important to follow the prescribed treatment plan consistently and be patient, as it may take several months for the new, healthy nail to grow in fully. Maintaining good foot hygiene, regularly trimming nails, and keeping the affected area dry can help prevent recurrence.
Bacterial Infections
Bacterial nail infections typically respond well to treatment with appropriate antibiotics. The type of antibiotic prescribed will depend on the specific bacteria causing the infection and the severity of the case. Oral antibiotics are often the first line of treatment for bacterial infections.
In cases where abscesses or pus-filled pockets have formed, a healthcare professional may perform a drainage procedure to remove the accumulated fluid. This procedure can help alleviate pain, facilitate healing, and promote the effectiveness of antibiotic treatment.
Following the prescribed course of antibiotics is crucial for a successful outcome. It’s important to complete the full course of medication, even if symptoms improve before the treatment period is over. Failure to complete the course may result in incomplete eradication of the infection and potential recurrence.
Conclusion
In conclusion, distinguishing between nail fungus and bacterial infections is crucial for effective treatment and recovery. Nail fungus, caused by fungi, and bacterial infections, caused by bacteria, present similar symptoms but require different approaches. While nail fungus typically thrives in warm and moist environments, bacterial infections can occur due to injuries or poor hygiene.